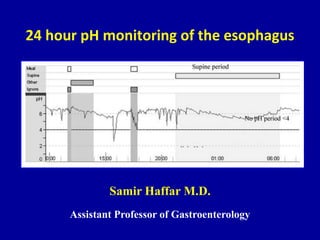
pH monitoring of the esophagus
- 1. 24 hour pH monitoring of the esophagus Samir Haffar M.D. Assistant Professor of Gastroenterology
- 2. pH monitoring of the esophagus Standard 24 hours pH monitoring Bravo capsule (tubeless capsule) Combined Multiple Intraluminal Impedance-pH (MII-pH)
- 3. Standard 24 hours pH monitoring of esophagus
- 4. Sites of 24 hour pH Monitoring • Single monitoring site: 5 cm above LES • Multiple monitoring sites: 5 & 20 cm above LES • One in the esophagus & one in proximal stomach • One or more in esophagus & another in hyopharynx
- 5. 5 cm above LES
- 6. Why 5 cm above LES? • Has been standard for many years • Chosen to avoid catheter migration into stomach • Moving by a 1 cm or two would not change results • Moving it 10 cm above LES miss a number of patients who are identified by the more distal location
- 7. Typical monitoring sites of 5 & 20 cm above manometrically determined LES
- 8. Location of LES • Manometric localization Reference method • pH step-up method Sudden rise to pH > 4 • LES locator Prior to pH • Fluoroscopic techniques Not accurate • Endoscoic technique Not accurate
- 9. Ideal pH electrode “No single probe meets all of these criteria” • Small • Firm enough • Rapid response time between pH 7 to pH 1 • Minimally affected by temperature • No hysteresis effect • No drift during 24 hours • Inexpensive • Simple to calibrate or disposable
- 10. Which pH Electrode ? Either can be used satisfactorily Glass electrodes Antimony electrodes 40 – 50 studies 10 studies Most linear response Most rapid response Less response fidelity Least recording drift Large diameter Smaller Siff bulky catheters More flexible Expensive Less expensive
- 11. Indications of Esophageal pH Recording • Normal endoscopic findings & reflux symptoms refractory to PPI • Endoscopy-negative patient before surgical anti-reflux repair • Patients suspected to have abnormal reflux after surgery • Refractory reflux in pts with chest pain after cardiac evaluation • Suspected ENT manifestations after failure of 4 weeks of PPI • GERD in an adult onset non-allergic asthma AGA Medical Position Statement. Gastroenterology 1996 ; 110 : 1981 - 96
- 12. No indications of esophageal pH recording • Esophageal pH recording not indicated to detect or verify reflux esophagitis (this is an endoscopic dg) • Esophageal pH recording not indicated to evaluate „„alkaline reflux‟‟ AGA Medical Position Statement. Gastroenterology 1996 ; 110 : 1981 - 1996
- 13. Why pH < 4? • Defined early in development of the technology • Its choice was based on: - Marked difference from normal esophageal pH of 7 - Pepsinogen converted to pepsin at pH 4 - pH < 4 was one that tends to produce symptoms • Some believe that drops in pH that do not reach level of 4.0 still may represent reflux that these events should also be used in calculations of indices
- 14. Composite scoring systems Johnson & DeMeester is the most commonly used Percentage of total time pH < 4 Percentage of upright time pH < 4 Percentage of supine time pH < 4 Number of reflux episodes Number of reflux episodes >5 min Longest reflux episode DeMeester score Normal < 14,72
- 15. Normal values of DeMeester’s score 50 healthy volunteers DeMeester TR et al. Ann Surg 1976 ; 184 :459 – 470.
- 16. Normal 24 hours esophageal pH monitoring Composite DeMeester score: 8.4 DeMeester normal < 14.72 (95th percentile) Bremner CG et al. Esophageal disease & testing. Taylor & Francis Group, 2005.
- 17. Typical distal & proximal 24 hour esophageal pH
- 18. Nocturnal acid breakthrough • Defined arbitrarily as intragastric pH < 4 for > 1 h overnight during administration of PPI • Occurs even on twice-daily therapy • Common enough: rule rather than exception • Not without controversy: little to do with reflux • Addition of H2RAs at bedtime to PPI bid controls NAB better than PPI therapy alone?
- 19. Nocturnal acid breakthrough Gastric pH < 4 for at least 1 h during the night in patients with persistent heartburn on standard dose PPIs twice daily Combined gastric & esophageal 24 hr pH monitoring
- 20. Qualitative analysis Symptom–reflux correlation • Symptom index: Positive if ≥ 50% • Symptom sensitivity index: Positive if > 10 % • Symptom association probability Positive if > 95% Determine relationship between heartburn episodes & acid reflux events, regardless if pH test is normal or abnormal
- 21. Symptom index Positive if 50 % or more Not take into account overall number of reflux episodes
- 22. Symptom Sensitivity Index Positive if 10 % Not take into account overall number of symptoms
- 23. Symptom Association Probability Calculation Positive if 95% • Divides tracing into 2-min segments & looks at whether a symptom & acid are present during each 2 minute segment • The analysis uses contingency table analysis of 4 possible outcomes for each segment: acid + symptom + acid + symptom – acid – symptom + acid – symptom –
- 24. Overall amount of acid exposure & number of reflux episodes are the focus of many studies using ambulatory pH testing Relationship between symptoms & esophageal acid is equally (or perhaps more) important
- 25. 24 hour pH esophageal monitoring On & off therapy • Off therapy Uncertainty about diagnosis of reflux Mildest grades of esophagitis: redness - friability Very short segments of BE • On therapy Patient who has failed a therapeutic trial Patient has known reflux or highly likely to have reflux pH probe in esophagus & another in stomach (NAB)
- 26. 24 hours pH monitoring & medications • PPI should be stopped for 5 – 7 days • Other medications should be stopped for 1 – 3 days • Patient must not use antacids or other OTC medications for duration of the study
- 27. Percentage of total time pH < 4 Normal values • Off therapy 5 cm above LES 20 cm above LES 1 % Periods of meals or acidic beverages excluded • On therapy 5 cm above LES 20 cm above LES ? * Based on 95% CI obtained in healthy subjects treated with omeprazole 40 mg qd Kuo B et al. Am J Gastroenterol 1996 ; 91 : 1532 – 8. 4 – 5.5 % 1.6 – 4 %*
- 28. Abnormal acid exposure time in heartburn Disease Percentage of total time pH < 4 Barrett‟s esophagus 93 % * ENRD: Endoscpic Negative Reflux Disease * *NERD: Non Erosive Reflux Disease Erosive esophagitis 75 % (in one study) ENRD* NERD** Functional heartburn - SI > 50% - SI < 50% 50 % 100 % 0 % Hypersensitive esophagus Non acid reflux or motor event 24 hr pH monitoring is not gold standard for diagnosis of GERD
- 29. Bravo capsule
- 30. Bravo system (Medtronics) Esophageal Probe 25 x 6 x 5.5 mm Battery pH electrode Suction chamber Radio transmitter Delivery system Receiver 100 x 70 x 30 mm - 165 g
- 31. Advantages of Bravo capsule • Better tolerance by patients • Fixed position of the capsule (6 cm above SCJ*) • Prolonged monitoring under more physiologic conditions (48 hours) * SCJ: squamocolumnar junction
- 32. Bravo normal values 50 asymptomatic volunteers 1st 24 h 2nd 24 h Mean (+ SD) 95th percentile Mean (+ SD) 95th percentile % total time at pH < 4 1.79 (2.16 5.89 1.78 (1.78) 5.64 % upright time at pH < 4 2.45 (3.14) 7.81 2.54 (2.57) 7.46 % supine time at pH < 4 0.37 (1.18) 1.58 0.34 (1.28) 1.29 Number of reflux episodes 21.2 (18.5) 55.30 22.3 (19.8) 56.15 No of reflux episodes >5 min 0.62 (1.21) 3.55 0.75 (1.15) 3.00 Longest reflux episode 3.79 (4.31) 11.23 5.95 (4.52) 17.03 DeMeester score 6.02 (4.82) 15.93 5.95 (4.52) 15.48
- 33. Conventional pH vs Bravo capsule Head to head comparison – 40 patients Bruley des Varannes S. Gut 2005 ; 54 ; 1682 – 1686.
- 34. Bravo capsule Causes of under-recording • Data drop-up • Short reflux event not recorded • Reflux events appear shorter
- 35. Bravo capsule Data drop-out Malfunctions in the electronics or the receiver Interpreted as artifact & not represented in final pH report Improved by 7 cm antenna & use of fiberglass Gastrointest Endoscopy Clin N Am 2005 ; 15 : 307 – 318.
- 36. Bravo capsule Short reflux events not recorded Bruley des Varannes S. Gut 2005 ; 54 ; 1682 – 1686.
- 37. Bravo capsule Reflux events appear shorter Bruley des Varannes S. Gut 2005 ; 54 ; 1682 – 1686.
- 38. Trouble shooting in Bravo capsule • Severe odynophagia & chest pain (5%) Chest radiography to exclude perforation Viscous lidocaine Endoscopic removal if symptoms continue • Capsule detachment • Failure to disloge Endoscopic removal similar to polypectomy
- 39. Bravo capsule Classic early detachment (10% of patients) Easily recognized during inspection of pH tracing Gastrointest Endoscopy Clin N Am 2005 ; 15 : 307 – 318. Sudden prolonged drop in pH represents capsule in stomach Sharp rise as capsule enters small intestine through pylorus
- 40. Endoscopic removal of Bravo capsule Gastrointest Endoscopy Clin N Am 2005 ; 15 : 307 – 318.
- 42. Principle of “MII” • 2 steel rings separated by isolator • Alternating-current generator to apply electrical PD • Circuit closed through electrical charges (ions) contained in structures surrounding the catheter Gastrointest Endoscopy Clin N Am 2005 ; 15 : 257 – 264.
- 43. Impedance scale Refluxate: High conductivity & low impedance Air: Low conductivity & high impedance Bremner CG et al. Esophageal disease & testing. Taylor & Francis Group, New York, 1st edition, 2005.
- 44. Advantages of MII • Content of refluxate Liquid – Gas – Mixed • Direction of bolus Anterograde – retrograde • Height of refluxate • pH characteristics Acid (combined MII-pH) Weekly acid Weekly alkaline Acid re-reflux
- 45. Liquid bolus Gastrointest Endoscopy Clin N Am 2005 ; 15 : 257 – 264. 1) Initial drop Liquid enters impedance-measuring segment 2) Rise Bolus cleared from this segment 3) Overshoot Decreased luminal cross-section during contraction 4) Return to baseline
- 46. Air bolus (Belch, Air swallow) 1) Rapid rise Presence of air bolus inside esophagus 2) Rapid decrease Air bolus clears from this segment Gastrointest Endoscopy Clin N Am 2005 ; 15 : 257 - 264.
- 47. Mixed air – liquid Bolus 1) Rapid Rise Air in front of the bolus 2) Rapid drop Liquid component of mixed bolus 3) Rise Liquid being cleared from this segment 4) Return to baseline Gastrointest Endoscopy Clin N Am 2005 ; 15 : 257 – 264.
- 48. Antegrade bolus movement (MII) Observed during swallowing Progression of impedance from proximal to distal Gastrointest Endoscopy Clin N Am 2005 ; 15 : 257 – 264.
- 49. Retrograde bolus movement (MII) Observed in reflux Progression of impedance from distal to proximal Gastrointest Endoscopy Clin N Am 2005 ; 15 : 257 – 264.
- 50. Combined MII • MII used clinically only in combination – With esophageal manometry (MII-EM) – With pH (MII-pH) • MII not considered as replacement for manometry & pH techniques but as complementary procedure that expands diagnostic potential of esophageal function testing & reflux monitoring
- 51. Combined MII-pH probe • Impedance orifices 3, 5, 7, 9, 15, & 17 cm from the tip • pH orifice 5 cm from the tip • MII-pH probe = pH probe Do not change patient comfort Bremner CG et al. Esophageal disease & testing. Taylor & Francis Group, NY, 1st edition, 2005.
- 52. “Sleuth” monitor – Sandhill “Sleuth” monitor attached to the catheter & worn around a belt during the recording period
- 53. GERD classification by combined MII-pH Acid reflux Reflux with drop of pH from above 4.0 to below 4.0 Superimposed acid reflux (Acid re-reflux) Acid reflux occurs while pH < 4.0 Weakly acidic reflux Reflux results in esophageal pH between 4.0 & 7.0 Weakly alkaline reflux Reflux with nadir esophageal pH does not drop < 7.0 Sifrim D et al. Gut 2004 ; 53 ; 1024 – 1031.
- 54. Acid reflux (MII-pH) Gastrointest Endoscopy Clin N Am 2005 ; 15 : 361 – 371.
- 55. GERD classification by combined MII-pH Acid reflux Reflux with drop of pH from above 4.0 to below 4.0 Superimposed acid reflux (Acid re-reflux) Acid reflux occurs while pH < 4.0 Weakly acidic reflux Reflux results in esophageal pH between 4.0 & 7.0 Weakly alkaline reflux Reflux with nadir esophageal pH does not drop < 7.0 Sifrim D et al. Gut 2004 ; 53 ; 1024 – 1031.
- 56. Superimposed acid reflux (MII-pH) Gastrointest Endoscopy Clin N Am 2005 ; 15 : 361 – 371.
- 57. GERD classification by combined MII-pH Acid reflux Reflux with drop of pH from above 4.0 to below 4.0 Superimposed acid reflux (Acid re-reflux) Acid reflux occurs while pH < 4.0 Weakly acidic reflux Reflux results in esophageal pH between 4.0 & 7.0 Weakly alkaline reflux Reflux with nadir esophageal pH does not drop < 7.0 Sifrim D et al. Gut 2004 ; 53 ; 1024 – 1031.
- 58. Weakly acidic reflux (MII-pH) Gastrointest Endoscopy Clin N Am 2005 ; 15 : 361 – 371.
- 59. GERD classification by combined MII-pH Acid reflux Reflux with drop of pH from above 4.0 to below 4.0 Superimposed acid reflux (Acid re-reflux) Acid reflux occurs while pH < 4.0 Weakly acidic reflux Reflux results in esophageal pH between 4.0 & 7.0 Weakly alkaline reflux Reflux with nadir esophageal pH does not drop < 7.0 Sifrim D et al. Gut 2004 ; 53 ; 1024 – 1031.
- 60. Weakly alkaline reflux (MII-pH) Gastrointest Endoscopy Clin N Am 2005 ; 15 : 361 – 371.
- 61. Recommendations for MII-pH monitoring • Endoscopy-negative patients with heartburn or regurgitation despite PPI & performed on PPI therapy • Utility of impedance in refractory reflux patients with chest pain or extraesophageal symptoms unproven • Current interpretation relies on SI, SSI or SAP • Therapeutic implications of abnormal test unproven ACG Practice Guidelines: Esophageal reflux testing. Am J Gastroenterol 2007 ; 102 : 668 – 685.
- 62. Advantages of 3 major types of pH testing pH Tubeless Combined MII-pH Comfort _ + _ Monitoring > 24 h _ + _ Nonacid reflux _ _ + Normal values + _ _ Proximal reflux + ? + Gastric monitoring + ? +
- 63. Thank You
Notas del editor
- Intragastric pH Monitoring:The evidence supporting the clinical significance and applicability of gastric pH monitoring is insufficient to recommend its routine use inclinical practice.Proximal pH Recording:available evidence does not support the routine use of proximal pH monitoring in clinical practice.
- Subgroups of Endoscopy-Negative reflux disease (ENRD)2 distinctive subgroups exist- Nonerosive reflux disease (NERD) Functional heartburnThese groups are separated by the presence or absence of abnormal levels of acid reflux.
- Therefore, pH recordings using the wireless pH system improve patients’ ability to perform their daily activities and thus provide a more accurate picture of their acid exposure profile as well as improve their compliance with the study.
- Using the wireless pH system, the 95th percentile for distal esophageal acid exposure for control subjects was 5.3%, a value higher than values reported in several although not all catheter-based system studies. The higher acid exposure threshold reported in healthy controls using the wireless pH system may be the consequence of less restriction in daily activities or the result of a thermal calibration error that existed in the pH catheter systems.The 48-h data could be interpreted using an average of the 2 days or only the 24-h period with the greatest acid exposure (worst day analysis). A significant increase in the sensitivity of pH testing and small decrease in specificity were evident when utilizingthe worst day data compared with either the initial 24-h or overall 48-h data in comparing controls with GERD patients.
- Strong correlation in esophageal acid exposure between 2 systemsCFS under recorded acid exposure
- Relatively new technique developed in early 1990s at Helmholtz Institute in Aachen (Germany)Silny* provided first description of this technique that assesses intraluminal bolus movement by measuring changes in conductivity of intraluminal content
- A recent, multicenter study examined the impedance characteristics of 60 healthy subjects during 24-h ambulatory monitoring. Based on impedance values 5 cm above the LES, the median number of total reflux episodes per 24 h was 30, the majority of which occurred in the upright position.Approximately two-thirds of the episodes were acid and another third weakly acidic reflux. Weakly alkaline reflux was distinctly uncommon in this healthy cohort. Similar frequencies were recently reported from a multicenter European study. References:Shay S, Tutuian R, Sifrim D, et al. Twenty-four hour ambulatory simultaneous impedance and pH monitoring: A multicenter report of normal values from 60 healthy volunteers. Am J Gastroenterol 2004;99:1037–43.Zerbib F, Bruley des Barannes S, Roman S, et al. 24 hour ambulatory esophageal multichannel intraluminal impedance-pH in healthy European subjects. Gastroenterology 2005;128:A396.