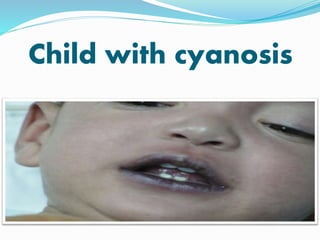
Child with cyanosis
- 2. Presented by : Group C4 5th year medical students Tripoli university Pediatric
- 3. Objectives Definition of cyanosis Types of cyanosis Causes of cyanosis Complications Management
- 4. Cyanosis is derived from the colour ‘cyan’, which comes from ‘kyanous’, the Greek word for blue . Definition: It is Bluish discoloration of skin and mucous membrane caused by increase concentration of reduced hemoglobin > 5g/dl so its not less pronounced if the child is anemic.
- 5. Types of cyanosis Peripheral Central
- 6. Peripheral cyanosis (blueness of hands &feet) Normal systemic arterial oxygen saturation. The increased extraction of oxygen results from sluggish movement of blood through the capillary circulation Sites Tip of nose Ear lobules Outer aspect of lips,chin,cheek Tips and nailbeds of fingers,toes Palms,soles Tongue is spared
- 7. Causes: vasoconstriction ( exposure to cold) polycythemia low cardiac output
- 8. Central cyanosis Pathologic condition caused by reduced arterial oxygen saturation. due oxygenation defect in lung or admixture of venous and arterial blood Involves highly vascularized tissues, through which blood flow is brisk . Cardiac output typically is normal, and patients have warm extremities. It is evident when O2 saturation falls below 90% From 90_95% (desaturated)
- 9. Sites: Tongue (margins & undersurface) Inner aspect of lips Mucous membranes of gums ,soft palate ,cheeks
- 11. Causes of central cyanosis 1_Respiratory disorders : upper airway obstruction Respiratory distress syndrome (RDS) Meconium aspiration(MAS) Pneumonia (sepsis) PPHN_Failure of pulm.vascular resistance to fall after birth Pulmonary hypoplasia Bronchopulmonary dysplasia(mechanical ventilation) Congenital diaphragmatic hernia Asthma
- 12. 2_CNS disorders: ICH Birth asphyxia Seizures Oversedation (direct or through maternal route)
- 13. 3_Cardiac disorders: Cyanotic congenital heart diseases (right to left shunt) 5Ts Tetralogy of Fallot (TOF) Transposition of great vessels(TGA) Total anomalous pulmonary venous return Truncus arteriosus Tricuspid atresia Note: persistant cyanosis in otherwise well infant is nearly always a sign of CHD
- 14. Ebstein malformation of the tricuspid valve Left hypoplastic heart Single ventricle Critical pulmonary atresia Heart failure/Cardiogenic Shock others Polycythemia Methemoglobinemia Metabolic diseases Infection _septicemia (physiological) : High altitude – Acrocyanosis “newborn”
- 15. cause example Cardiovascular disorders congenital cyanotic heart disease Respiratory disorders - Pneumonia - Bronchiolitis - RDS & meconium aspiration - Pneumothorax & pleural effusion 0CNS disorders - intra cranial hemorrhage0 - Tonic clonic seizure hematological disorders - Methemoglobinemia - Polycythemia - Congenital cyanosis other disorders - High Altitude - hypothermia - obstructive sleep apnea
- 16. Differential Cyanosis Hands red (less blue) and feet blue seen in PDA with reversal of shunt (Differential Cyanosis) Requires pulmonary vascular resistance elevated to a systemic level and a patent ductus arteriosus Left to right sunt pulmonary HT reversed shunt (Rt Lt shunt) Desaturated blood from the ductus enters the aorta distal to the left subclavian artery, sparing the brachiocephalic circulation.
- 17. Management Aim: * Differentiate physiologic from pathologic cyanosis * Differentiate cardiac from non- cardiac cause of cyanosis * Find causes which needs urgent treatment or referral
- 18. Do : 1_complete maternal and newborn history 2_perform a full physical examination 3_ Investigation
- 19. Investigation * Pulse oximetry: (normal O2 sat. ≥ 95%) * ABGs : PaO2: to confirm central cyanosis ↑ PaCO2: may indicate pulmonary or CNS disorders. ↓ pH: sepsis, circulatory shock, severe hypoxemia * Hyperoxia test (Is it due cardiac or pulmonary cause?) placing the infant in 100% oxygen for 10 minutes. If he remains cyanotic after this period, the cyanosis is said to be secondary to cyanotic heart diseases(SaO2 not reach the normal value).
- 20. * CBC : ↑ or ↓ WBC : sepsis Hematocrit > 65% : polycythemia * Methemoglobinemia : ↓ SaO2, normal PaO2, chocolate-brown blood , HB-M * Sepsis screening * ECG: Dx for Tricusped atresia (Lt axis deviation only is seen) * Echo: Dx for CHD * Chest x-ray
- 21. Treatment * Warming of the affected area: in peripheral cyanosis * Oxygenation & adequate ventilation (PaO2 normalizes completely during artificial ventilation in infant with CNS disorder) * IV fluids Children who have difficulty in feeding due to cyanosis need fluids to be administrated. * If sepsis is suspected or another specific cause is not identified, start on broad spectrum antibiotics then obtain a full septic screening
- 22. * Drugs: Prostaglandin E1 For ductal dependent CHD IV Infusion of PGE1 at a dose of (0.05- to maintain patency 0.1mcg/kg/min) S/E- hypoventilation, apnea, edema and low grade fever * Surgery
- 23. CCHD
- 25. Tetralogy of Fallot Boot shape
- 26. Total Anomalous Pulmonary Venous Return(TAPVR) Snowman
- 27. Transposition of Great Arteries Egg on a string
- 30. Complication of CCHD Stunt of growth Cyanotic spells (in TOF) brain abscess Cerebral thrombosis (CVA) pulmonary TB (oligemic lung) HF “rare” Death
- 31. Tx of cyanotic spells: Hold the baby in knee chest position O2 Morphine (subcut.) : to relieve pain & anexiety NaHco3 : for metabolic acidosis Inderal (Beta blocker) : prevent recurrent attack
- 32. Thank you
Notas del editor
- Tonic clonic type of convulsion
- Newborn cyanotic at birth when transfer from intrauterine to extrauterine life , so need quick warming &dryness
- As : physiological Cyanosis soon after birth-normal transition from intrauterine to extrauterine life History of convulsion & general depression ,shallow, irregular respirations and periods of apnea strongly suggest CNS problem
- Pneumonia/ sepsis- PROM Foul smelling liquor Maternal pyrexia Maternal GBS TTN – Birth by cesarean section with or without labor Male sex Family history of asthma (especially in mother) Macrosomia Maternal diabetes Polycythemia- small-for-gestational age MAS- Post maturity Small for gestational age Placental dysfunction Fetal distress Meconium stained liquor Pneumothorax- Aggressive resucitation IPPV Meconiun aspiration HMD Hypoplastic lung Staph pneumonia Hyaline membrane disease- Premature infant Infant of diabetic mother
- CHD= Cyanotic heart diseases SaO2= oxgen saturation
- Brain abscess becos. Blood from Rt to Lt without pass to lung which has a phagocytic activity (filter bld) so go to the brain & cause abscess if contain organisms