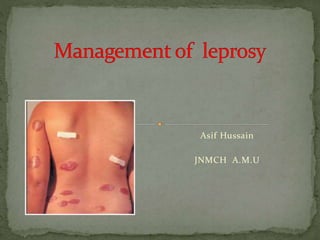
Management of Leprosy
- 1. Asif Hussain JNMCH A.M.U
- 2. LEPROSY IS A CHRONIC GRANULOMATOUS INFECTION CAUSED BY MYCOBACTRIUM LEPRAE (By G.A.Hansen 1873) SKIN PERIPHERAL NERVOUS SYSTEM UPPER RESPIRATORY TRACT EYES TESTES M.Leprae has uniqe tropism for peiphral nerves Reactional state responsible for morbidity & disease if not treated leads to charecterstic deformity & profound social stigma
- 3. First bacterium to be identified as causing disease in humans. Obligate intracellular bacilli Acid-fast Reductive evolution Cell wall contains PGL-1, Trisaccharides Grows in cooler tissues Doubling time 14 days Culture Incubation period
- 4. EPIDEMIOLOGY Disease of developing world Endemic among 10 to 15 million people living in poor tropical countries. Prevalence rate decreased from 21 cases/ 10000 population in 1985 to <1 per 10000 in 2000. Leprosy has been eliminated from 119 of 122 countries where it was considered as a public health problem. 2005 - Elimination of Leprosy at National Level
- 5. M.leprae replicates intracellularly in the skin histocytes and nerve cells and has two forms. Tuberculoid, which induces a cell-mediated response that limits its growth. M.leprae multiplies at the site of entry, (skin), invading and colonizing Schwann cells. The microbe then induces T-helper lymphocytes, epitheloid cells, and giant cell infiltration of the skin, causing infected individuals to exhibit large flattened patches with raised and elevated red edges on their skin. These patches have dry, pale, hairless centers, accompanied by a loss of sensation on the skin. The loss of sensation may develop as a result of invasion of the peripheral sensory nerves.
- 6. The second form is the lepromatous form. This form of the microbe proliferates within the macrophages at the site of entry. It also grows within the epithelial tissues of the face and ear lobes. With cell mediated immunity impaired, large numbers of M.leprae appear in the macrophages and the infected patients develop papules at the entry site, marked by a folding of the skin. Gradual destruction of cutaneous nerves lead to what is referred to as "classic leonine facies." Extensive penetration of this microbe may lead to severe body damage; for example the loss of bones, fingers, and toes.
- 8. Ridley Jopling Tuberculoid (TT) Borderline tuberculoid (BT) Borderline (BB) Borderline Lepromatous (BL) Lepromatous (LL). W.H.O Multibacillary (MB) Paucibacillary (PB) Single skin lesion paucibacillary
- 10. Physical examination findings and skin biopsy and/or smear. Lepromin test. Antibody against phenolic glycolipid antigen. PCR
- 11. Early reaction: (Fernandez) An inflammatory response develops within 24 to 48 hrs. & tends to disappear after 3 to 4 days. +ve test if the diameter of red area is more than 10mm at the end of 48 hrs. It indicates whether person has previously sensitized by exposure to & infection by leprosy.
- 12. Late Reaction: (Mitsuda) This reaction becomes apparent in 7-10days and reaching its maximum in 3 or 4 weeks. Test is read at 21 days and at the end, if nodule is more than 5mm in diameter reaction is said to be (+)ve. The nodule may even ulcerate & heal with scarring.
- 13. Leprosy reactions are the acute episodes of inflammation occurring during the chronic course of disease. They pose a challenging problem because they increase morbidity due to nerve damage even after the completion of treatment.
- 15. Dapsone Clofazimine Rifampicin Ofloxacin Minocycline
- 16. Diamino diphenyl sulfone. Structural analogs of PABA – prevents Folic acid synthesis. Competitive inhibitor of dihydropteroate synthase. Resistance - mutant genes encoding dihydropteroate synthase Oral bioavailability.
- 18. Hemolysis in patients with G6PD deficiency. nervousness, insomnia, blurred vision, paresthesias, drug fever, pruritus, psychosis, and a variety of skin rashes.
- 19. Fat soluble Riminophenazine dye. MOA - Bind to DNA of M. leprae, membrane disruption, inhibition of mycobacterial phospholipase A2, inhibition of microbial K+ transport, generation of hydrogen peroxide, interference with the bacterial electron transport chain. Variable oral bioavailability. Hydrolytic dehalogenation, hydrolytic deamination, glucuronidation, and hydroxylation.
- 20. AE – Acute abdominal symptoms, Skin discolouration. Anti-inflammatory effects via inhibition of macrophages, T cells, neutrophils, and complement. Interaction
- 21. Semisynthetic derivative of macrocyclic antibiotic rifamycin. Rapidly bactericidal against M. leprae. β subunit of DNA-dependent RNA polymerase - RNA transcription. It is readily absorbed with an elimination half-life of ~3 hours. Excreted mainly through liver into bile and undergoes enterohepatic circulation. Enzyme inducer – Auto enzyme induction, Ocp’s, warfarin. Resistance
- 22. Adverse Effects Rash, fever, and nausea and vomiting. Hepatitis, Hemolysis, hemoglobinuria, Flu like syndrome Orange-tan discoloration of skin, urine, feces, saliva, tears.
- 23. Patients with intolerance, resistance, or clinical failure to primary therapy(rifampicin). Inhibits DNA gyrase - DNA replication and transcription. 400mg on first day followed by 200mg/day.
- 24. Intolerance to Clofazimine. 30S ribosomal subunit. 100mg/day. Deposit in tooth enamel and discolor teeth.
- 25. Multi drug therapy (MDT) is a key element for cure. MDT is available free of charge from WHO The drugs used in WHO-MDT are a combination of Rifampicin,clofazimine and Dapsone for MB leprosy patients Rifampicin and Dapsone for PB leprosy patients. Treatment of leprosy with only one anti leprosy drug will always result in development of drug resistance. Treatment with Dapsone or any other anti leprosy drug used as monotherapy should be considered as unethical practice.
- 28. Type 1 reaction: Clofazimine 200 mg daily Corticosteroids Loss of sensation or other peripheral nerve symptoms, corticosteroids should be started immediately to prevent permanent damage. Type 2 reactions may not respond to corticosteroids alone, and the addition of drugs such as thalidomide.
- 29. 40 mg (8 tablets) every morning for 14 days 30 mg (6 tablets) every morning for 14 days 20 mg (4 tablets) every morning for 14 days 15 mg (3 tablets) every morning for 14 days 10 mg (2 tablets) every morning for 14 days 5 mg (1 tablets) every morning for 14 days Aspirin or paracetamol as required Examine the patient every 14 days before reducing the dose Continue MDT
- 30. Reduce systemic concentrations of TNF-α, IL-2, Interferon 100–300 mg/day Avoided in pregnancy and during lactation.
- 31. Care of hands-avoid direct skin contact with hot objects. While working reducing pressure prevents injuries. Gentle massage keeps fingers mobile. Exercise to keep hands mobile. Use clothes or canvas gloves for protection. Care of feet-clean & soak in salt water for 15 min. Rub off hard skin with water. Rest the swollen foot by elevation. Regular dressing helps to heal simple ulcer. Use MCR (micro-cellular rubber insole) footwear to prevent injuries.
- 32. THANK YOU!
