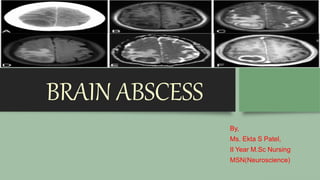
Brain abscess
- 1. BRAIN ABSCESS By, Ms. Ekta S Patel, II Year M.Sc Nursing MSN(Neuroscience)
- 2. Introduction: • A brain abscess is a collection of pus enclosed in the brain tissue, caused by a bacterial or fungal infection.
- 3. • Brain abscess (or cerebral abscess) is an abscess caused by inflammation and collection of infected material, coming from local (ear infection, dental abscess, infection of paranasal sinuses, infection of the mastoid air cells of the temporal bone, epidural abscess) or remote (lung, heart, kidney etc.) infectious sources, within the brain tissue.
- 4. • The infection may also be introduced through a skull fracture following a head trauma or surgical procedures. • Brain abscess is usually associated with congenital heart disease in young children. It may occur at any age but is most frequent in the third decade of life.
- 5. Definition: • Brain abscess is defined as purulence and inflammation in one or more localized regions within the brain parenchyma.
- 6. Causes and risk factors: • Nearly anyone can get a brain abscess, but certain groups of people are at a higher risk than others. Some diseases, disorders, and conditions that raise your risk include:
- 7. • A compromised immune system due to HIV or AIDS • Cancer and other chronic illnesses • Congenital heart disease • Major head injury or skull fracture
- 8. • Meningitis • Immunosuppressant drugs, such as those used in chemotherapy • Chronic sinus or middle ear infections
- 9. Sign and symptoms • Symptoms may develop slowly, over a period of 2 weeks, or they may develop suddenly. They may include:
- 10. 1. Changes in mental status • Confusion
- 12. • Drowsiness
- 13. • Eventual coma
- 14. • Inattention
- 15. • Irritability
- 16. • Slow thought processes
- 17. 2. Decreased movement 3. Decreased sensation 4. Decreased speech (aphasia) 5. Fever and chills 6. Headache
- 18. 7. Language difficulties 8. Loss of coordination 9. Loss of muscle function, typically on one side 10. Seizures 11. Stiff neck 12. Vision changes 13. Vomiting
- 19. Diagnostic evaluation: • A brain and nervous system (neurological) exam will usually show signs of increased intracranial pressure and problems with brain function. • Tests to diagnose a brain abscess may include: • Blood cultures
- 20. • Chest x-ray • Complete blood count (CBC) • Head CT scan • Electroencephalogram (EEG) • MRI of head • Testing for the presence of antibodies to organisms such as Toxoplasma gondii and Taenia solium
- 21. • A needle biopsy is usually performed to identify the cause of the infection.
- 22. Treatment: • A brain abscess is a medical emergency. Pressure inside the skull may become high enough to be life threatening. Patient need to stay in the hospital until the condition is stable. Some people may need life support.
- 23. Medication, not surgery, is recommended if patient have: • Several abscesses (rare) • A small abscess (less than 2 cm) • An abscess deep in the brain • An abscess and meningitis • Shunts in the brain for hydrocephalus (in some cases the shunt may need to be removed temporarily or replaced)
- 24. • Toxoplasma gondii infection in a person with HIV
- 25. • Antibiotics will be prescribed. Antibiotics that work against a number of different bacteria (broad spectrum antibiotics) are most commonly used.
- 26. • Antifungal medications may also be prescribed if the infection is likely caused by a fungus. • Immediate treatment may be needed if an abscess is injuring brain tissue by pressing on it, or there is a large abscess with a large amount of swelling around that it is raising pressure in the brain.
- 27. Surgery is needed if: • Increased pressure in the brain continues or gets worse • The brain abscess does not get smaller after medication • The brain abscess contains gas (produced by some types of bacteria) • The brain abscess might break open (rupture)
- 28. • Surgery consists of opening the skull, exposing the brain, and draining the abscess. Laboratory tests are often done to examine the fluid. This can help identify what is causing the infection, so that more appropriate antibiotics or antifungal drugs can be prescribed.
- 29. • The surgical procedure used depends on the size and depth of the abscess. The entire abscess may be removed (excised) if it is near the surface and enclosed in a sac.
- 30. • Needle aspiration guided by CT or MRI scan may be needed for a deep abscess. During this procedure, medications may be injected directly into the mass. • Certain diuretics and steroids may also be used to reduce swelling of the brain.
- 31. Prognosis: • If untreated, a brain abscess is almost always deadly. With treatment, the death rate is about 10 - 30%. The earlier treatment is received, the better. • Some patients may have long-term neurological problems after surgery.
- 32. Complications: • Brain damage • Meningitis that is severe and life threatening • Return (recurrence) of infection • Seizures
- 33. Nursing Management & Interventions • Nursing interventions should support the medical treatment, as do patient teaching activities that address neurosurgical procedures.
- 34. • Patients and families need to be advised of neurologic deficits that may remain after treatment (hemiparesis, seizures, visual deficits, and cranial nerve palsies).
- 35. • Frequently assess neurologic status, especially LOC, speech and sensorimotor and cranial nerve functions. • WOF signs of increased ICP: decreased LOC, vomiting, abnormal pupil response and depressed respirations.
- 36. • The nurse assesses the family’s ability to express their distress at the patient’s condition, cope with the patient’s illness and deficits, and obtain support. • Always provide safety measures.