Placenta & Amnion (General Embryology)
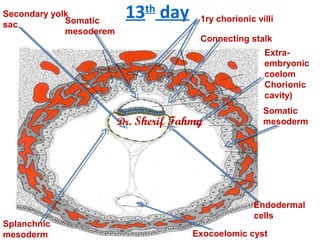
- 1. 13th day Endodermal cells Secondary yolk sac Exocoelomic cyst Somatic mesoderm Connecting stalk Somatic mesoderem Splanchnic mesoderm 1ry chorionic villi Extra- embryonic coelom Chorionic cavity) Dr. Sherif Fahmy
- 2. 13th day Somatic mesoderm Connecting stalk 1ry chorionic villi Cyto- trophoblast Intervillous space Syncytio- trophoblast Dr. Sherif Fahmy
- 3. Tertiary Chorionic Velli Dr. Sherif Fahmy Syncytio- trophoblast Cyto- trophoblast Somatic extraembryoni c mesoderm Fetal blood vessels Dr. Sherif Fahmy
- 4. Types of Tertiary Chorionic Velli
- 5. Decidua basalis (Decidual plate) Chorion frondosum Chorionic plate Chorion leave Dr. Sherif Fahmy
- 6. Fetal Membranes Dr. Sherif Fahmy
- 7. Fetal membranes: 1- Chorion and placenta. 2- Amnion. 3- Umbilical cord. 4- Yolk sac. Dr. Sherif Fahmy
- 9. It is the wall of chorionic vesicle. Time: Chorionic vesicle is formed at the 12th day by the formation of extra-embryonic mesoderm. Structure of chorion: 1- Syncytiotrophoblast. 2- Cytotrophoblast. 3- Somatic extra-embryonic mesoderm. Chorionic velli: 1- Primary. 2- Secondary. 3- Tertiary. Dr. Sherif Fahmy
- 10. Somatic mesoderm Connecting stalk Secondary yolk sac Somatic mesoderm Extra-embryonic coelom Amniotic cavity Splanchnic mesoderm Syncytio- trophoblast Cyto- trophoblast Chorion Exocoelomic cyst Embryonic disc Chorionic Vesicle Dr. Sherif Fahmy Endodermal cells Dr. Sherif Fahmy Dr. Sherif Fahmy
- 11. Dr. Sherif Fahmy Primary chorionic villus Cyto- trophoblast Syncytio- trophoblast Dr. Sherif Fahmy
- 12. Dr. Sherif Fahmy Syncytio- trophoblast Cyto- trophoblast Somatic mesoderm Secondary chorionic villus Dr. Sherif Fahmy
- 13. Dr. Sherif Fahmy Syncytio- trophoblast Cyto- trophoblast Mesoderm Fetal blood vessels Tertiary chorioniv villus
- 14. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 15. 1- Primary chorionic velli (start of 3rd week): cyncytiotropholblasts and cytotrophoblast. 2- Secondary chorionic velli (middle of 3rd week): Cyncytiotrophoblast, cytotrophoblast and mesoderm (in the central core). 3- Tertiary chorionic velli (end of 3rd week): formation of fetal blood vessels in the mesoderm. -Tertiary velli, opposite decidua basalis form side branches and called chorion frondosum while under decidua capsularis it will degenerates to form chorion leave. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 17. Morphology of Placenta • It is the organ of exchange of materials between fetal and maternal blood. • Shape: Disc like. • Surfaces: • -Fetal surface: It is covered with amnion and fetal blood vessels. Umbilical cord is attached near the center of this surface. • -Maternal surface: Shows 15 – 20 rounded elevations (cotyledons) with septa inbetween). • Diameter: 15 -25 cm. • Thickness: About 3 cm. • Weight: About 500 – 600 gm • Site: At original implantation site which is upper part of posterior wall of uterus. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 18. Cotyledon Groove between cotyledons Umbilical cord Maternal surface Dr. Sherif Fahmy Dr. Sherif Fahmy
- 19. Fetal surface covered with amnion Umbilical cord Dr. Sherif Fahmy Dr. Sherif Fahmy
- 21. Dr. Sherif Fahmy
- 22. Dr. Sherif Fahmy
- 24. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 25. Decidua basalis Arteriol Venule Decidual septum Cytotrophoblastic shell Decidual plate Stem villous Floating velli Intervillous space Chorionic plate Umbilical veinUmbilical artery Amnion Mesoderm Syncytiotrophoblast Cytotrophoblast Dr. Sherif Fahmy
- 26. Structure of Placenta • The placenta is developed from 2 parts: Chorion frondosum (tertiary velli) and Decidua basalis. The internal structure of placenta is described as follow: • 1- Chorionic velli: They are stem and absorbing (floating). They are composed of syncytiotrophoblast, cytotrophoblast, mesoderm and fetal blood vessels. • 2- Intervillous spaces: They are spaces between stem villi that are filled with maternal blood. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 27. 3- Cytotrophoblastic shell; complete sheet of cytotrophoblastic cells that is present between decidua basalis and intervillous spaces. 4- Decidual septa: They descend from roof of intervillous spaces. Each septum is composed of decidua basalis, cytotrophoblast and cyncytiotrophoblasts. There is a groove opposite each septum which are separated from each other by cotyledones. 5- Chorionic plate: composed of amnion, extraembryonic mesoderm,cytotrophoblast and syncytiotrophoblast. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 28. 6- Decidual plate: composed of: - Syncytiotrophoblast. - Cytotrophoblast. - Decidua basalis. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 29. Placental barrier: It is the separation between fetal and maternal blood. Structure: 1- Syncytiotrophoblast. 2- Cytotrophoblast. 3- Extraembryonic mesoderm. 4- Endothelium of fetal blood vessels. Functions of the barrier: 1- Separates between fetal and maternal blood. 2- Permites gaseous and nutritive exchange. 3- Prevents passage of bacteria, most viruses and damaging factors. Disappear in 2nd ½ of pregnancy Dr. Sherif Fahmy Dr. Sherif Fahmy
- 30. Placental circulation: 1- Maternal part: Maternal blood flow from endometrial arterioles to the intervillous spaces where floating velli are bathed in maternal blood. Exchange of gases and nutritive materials occurs. Then blood flows back from chorionic plate to endometrial veins. 2- Fetal part: umbilical arteries carry venous blood of the fetus to placenta while umbilical veins carry blood loaded with nutritive material and oxygen. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 31. Functions of placenta 1- Exchange of gases and metabolites. 2- Transmission of maternal antibodies starting from 14th week. 3- Production of hormones as progesterone, estrogen, HCG and somatomammotropin 3- Barrier against bacteria and most of viruses. 4- Excretory function as it excretes urea and creatinine. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 32. Anomalies of Placenta 1- Abnormalities in position: A- Placenta previa parietalis. B- Placenta brevia marginalis. C- Placenta brevia centralis. 2- Abnormality in shape: A- biloped placenta. B- Triloped placenta. 3- Abnormality in number: A- Twin placenta. B- Accessory placenta. 4- Abnormality in attachement of umbilical cord: A- Velamentous. B- Battle door. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 33. Placenta previa Marginalis & parietalis Dr. Sherif Fahmy Dr. Sherif Fahmy
- 34. Placenta previa centralis Dr. Sherif Fahmy Dr. Sherif Fahmy
- 35. Velamentous placenta Dr. Sherif Fahmy Dr. Sherif Fahmy
- 36. Battle door placenta Dr. Sherif Fahmy Dr. Sherif Fahmy
- 37. Accessory placenta Dr. Sherif Fahmy Dr. Sherif Fahmy
- 38. Placenta acreta Placenta percreta Dr. Sherif Fahmy Dr. Sherif Fahmy
- 39. AMNION
- 40. Dr. Sherif Fahmy Extraembryonic coelom (Chorionic Cavity) Dr. Sherif Fahmy
- 41. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 42. AMNION -It is a membrane that enclose amniotic cavity. -Formation: -It is formed at the 8th day as a small cavity in epiblast cells with formation of amnioblasts. -So, floor of the cavity is epiblast while the roof is formed from amnioblasts. -By the 12th day it becomes separated from cytotrophoblasts by primary mesoderm (Extraembryonic). -Amnio-ectodermal junction is at the margin of oval embryonic disc at the 3rd week.Dr. Sherif Fahmy Dr. Sherif Fahmy
- 43. 8th day of pregnancy Dr. Sherif Fahmy Endometrium Syncytio- trophoblast CytotrophoblastBlastocele Amnioblast Amniotic cavity Epiblast Hypoblast Trophoblast Dr. Sherif Fahmy
- 44. 9th & 10th days Dr. Sherif Fahmy Cyto- trophoblast Amnioblast Amniotic cavity Epiblast Hypoblast Heuser’s membrane Primary yolk sac Fibrin clot Dr. Sherif Fahmy
- 45. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 46. -At 3rd month amnion comes in contact with chorion to form amnio-chorionic membrane with obliteration of chorionic cavity. -By the end of 3rd month, uterine cavity is obliterated due to expansion of amniotic cavity. -Finally, the amniotic cavity surrounds the fetus and forms a tubular sheath around the umbilical cord. -Expansion of amniotic cavity leads to folding of the embryonic disc and amnio-ectodermal junction will be present at primitive umbilical ring. Dr. Sherif Fahmy
- 47. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 48. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 49. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 50. Dr. Sherif Fahmy Extraembryonic coelom (Chorionic Cavity) Dr. Sherif Fahmy
- 51. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 52. Dr. Sherif Fahmy Decidua basalis Decidua parietalis Decidua capsularis Chorion frondosum Uterine cavity Amniotic cavity Chorion frondosum Fused decidua parietalis and capsularis Amniotic cavity Decidua basalis Chorionic cavity Dr. Sherif Fahmy
- 53. Amniotic fluid - Normal volume is 1000 – 1500 cc clear watery fluid. - Source: 1st from amnioblast then from kidney. - If the volume is less than 500 cc it is called oligohydramnios. -If the volume is more than 2000 cc is called polyhydramnios. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 54. Functions of amniotic fluid: 1- At early pregnancy: 1- Acts as water cushion that absorbs external shocks. 2- Acts as heat insulator. 3- Prevents adhesion of embryo to wall of uterus. 4- Prevents adhesion of fetal parts. 2- At late pregnancy: 1- A space for accumulated urine. 2- Allows fetal movements to help body muscles to develop. 3- Help suckling training and development of gut muscles. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 55. 3- During labor: 1- Protects against uterine contractions. 2- Formation of bag of water that gradually dilate the cervix. 3- Sterile amniotic washes vagina before passage of baby. 4- Rupture of amniotic sac is a sign of start of delivery. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 56. Abnormalities of amniotic fluid: 1- Polyhydramnios. Causes: 1- No cause (35 %). 2- Maternal diabetes. 3- Congenital malformation e.g. anencephaly and esophageal atresia. 2- Oligohydramnios. Cause: -Renal agenesis. Dr. Sherif Fahmy Dr. Sherif Fahmy
- 57. YOLK SAC
- 58. Fate & development of yolk sac • Primary yolk sac: It replaces cavity of blastocyst after the formation of Heuser’s membrane which is formed of flat cells that originate from hypoblast cells at 9th & 10th day. • Secondary yolk sac: additional cells from hypoblast cells will line the Heuser’s membrane, reduction of size of yolk sac and formation of allantois. This occurs in the 13th day. • Defenitive yolk sac: During 3rd week, hypoblast become replaced by endoderm. After folding, it shares in formation of gut and the part remains outside the embryo is called defenitive yolk sac. It is connected to yolk sac by vitello-intestinal duct. Dr. Sherif Fahmy
- 59. 7th day: Dr. Sherif Fahmy Dr. Sherif Fahmy
- 60. 8TH Day of Pregnancy Endometrium Cytotrophoblasts Hypoblasts Amniotic cavity Epiblast Dr.Sherif Fahmy Dr. Sherif Fahmy
- 61. 9th & 10th days Primary yolk sac Heuser’s membrane Syncytio- trophoblast Hypoblast Amniotic cavity Epiblast Cyto- trophoblast Dr. Sherif Fahmy
- 62. 13th day Endodermal cells Secondary yolk sac Exocoelomic cyst Connecting stalk Splanchnic mesoderm Extra- embryonic coelom Chorionic cavity) Dr.Sherif Fahmy Chorionic Vesicle Dr. Sherif Fahmy
- 64. Dr. Sherif Fahmy
- 65. Functions of yolk sac: • Gut: foregut, midgut and hindgut. • Allantois: forms part of urinary bladder. • Primordial germ cells: Which are spermatogonia and oogonia which are formed in its caudal part (hind gut). • Vitelline vessels: develop from mesoderm around vitelline duct. Intra-embryonic part form portal vein and arteries of intestine. • Blood cells: develop in the mesoderm around the yolk sac. Dr. Sherif Fahmy
- 66. Abnormalities of Yolk Sac • 1- Vitelline cyst and fistula due to persistence of vitelline duct. • 2- Urachal cyst and fistula due to persistence of urachus from allantois. Dr. Sherif Fahmy
- 67. Dr. Sherif Fahmy
- 68. Dr. Sherif Fahmy